Glaucoma Treatment in Gettysburg & York
What is Glaucoma?
Glaucoma is a disease of the optic nerve, the nerve the connect the eye to the brain. The optic nerve is made up of many nerve fibers (like an electric cable with its numerous wires). Glaucoma damages nerve fibers, which can cause blind areas and vision loss.
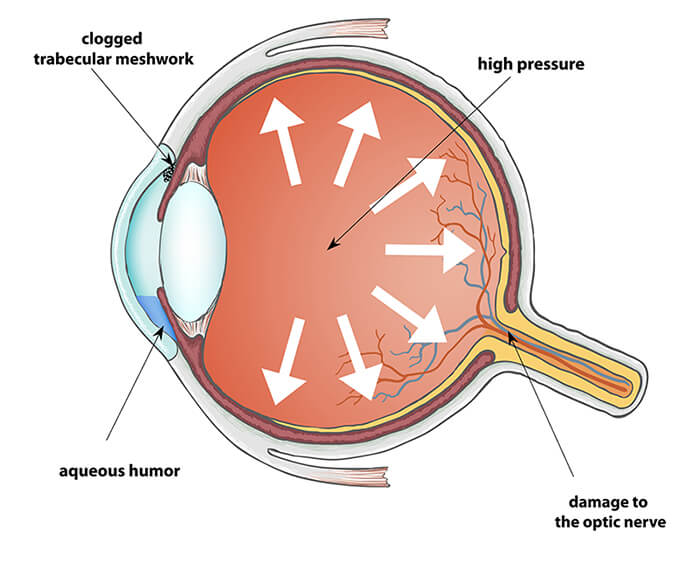
Glaucoma can be thought of as pressure damage to the optic nerve. Usually, in glaucoma the pressure within the eye (“intra-ocular pressure” or IOP) is higher than average, but glaucoma can occur at any IOP. The eye produces a clear fluid called “aqueous humor,” and a tiny drain at the base of the cornea drains that fluid out of the eye.
The usual reason for a pressure build-up is a partial blockage of the drain. Why a given IOP causes glaucoma damage in one person’s eye but not another’s remains a bit of a mystery
What are the types of Glaucoma?
Primary open-angle glaucoma
The most common form of glaucoma is primary open-angle glaucoma. In medicalese “primary” means “we don’t know what causes it.” Most people who develop primary open-angle glaucoma notice no symptoms until their vision is permanently impaired, which is why it is so important to get regular eye exams with dilation of the pupils.
Ocular hypertension is a risk factor for actual open-angle glaucoma. When the eye’s pressure is above normal, the risk of developing glaucoma increases. Several risk factors will affect whether you will develop glaucoma, including the level of IOP, family history of glaucoma, certain medical conditions, race and corneal thickness (people with thin corneas are more glaucoma-prone). If your risk is high, your ophthalmologist (Eye M.D.) or optometrist may recommend treatment to lower your IOP to prevent future damage.
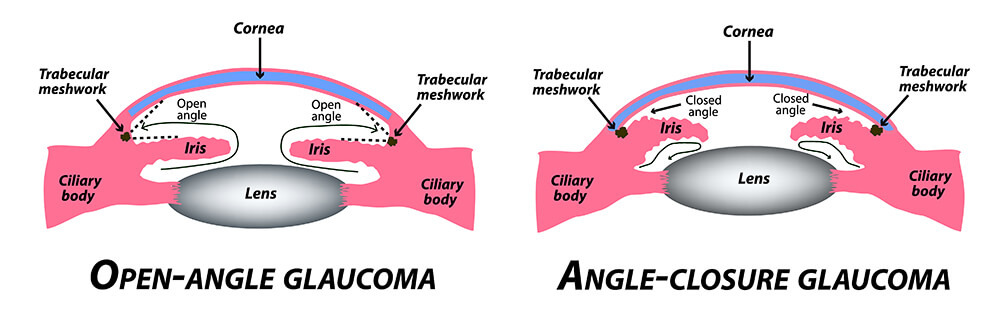
Angle-closure glaucoma
In angle-closure glaucoma, the iris (the colored part of the eye) may come forward and completely close off the drain, blocking the flow of aqueous fluid and leading to increased IOP and optic nerve damage. In “acute” angle-closure glaucoma there is a sudden increase in IOP to a very high level, due to rapid buildup of aqueous fluid. This condition is an emergency, because optic nerve damage and vision loss can occur within hours. An acute attack is characterized by dull eye pain with nausea, redness and blurred, misty vision with rainbows or haloes. Angle-closure glaucoma is more often “chronic”, that is, slow in onset. An eye exam will reveal this type of glaucoma. Angle closure glaucoma is usually treated by putting a hole in the iris with a laser. This is a simple office procedure.
Even some people with “normal” IOP can experience vision loss from glaucoma. This condition is called normal-tension glaucoma. In this type of glaucoma, the optic nerve sustains pressure damage, even though the IOP is considered statistically normal. Normal-tension glaucoma is not well understood, but lowering IOP has been shown to slow progression of this form of glaucoma.
Your doctor may tell you that you are at risk for glaucoma, if you have one or more risk factors, including having an elevated IOP, a family history of glaucoma, certain optic nerve conditions, or are of a particular ethnic background. People of African descent are prone to open-angle glaucoma; east Asians are prone to the angle-closure variety. Regular examinations with your eye doctor are important so that glaucoma doesn’t go undetected.
The goal of glaucoma treatment is to lower your eye pressure to prevent or slow further vision loss. Your doctor will recommend treatment, if the risk of vision loss is high. Treatment usually consists of laser treatment to make the eye’s drain work better and/or eye drops. Sometimes, surgery in the operating room is required to create a new drain in the eye. Glaucoma is a chronic disease that can be controlled but not cured. Ongoing monitoring (every three to six months) is needed to watch for changes and to be sure the IOP remains adequately low.

