Glaucoma Treatment in York
 The idea behind treating glaucoma is to lower the eye’s pressure, so that no more damage to the optic nerve occurs, preventing further vision loss. The only way we know to decrease the risk of further damage is to lower the eye’s intraocular pressure, the fluid pressure inside the eye. We can lower the pressure with laser, drops or surgery in the operating room.
The idea behind treating glaucoma is to lower the eye’s pressure, so that no more damage to the optic nerve occurs, preventing further vision loss. The only way we know to decrease the risk of further damage is to lower the eye’s intraocular pressure, the fluid pressure inside the eye. We can lower the pressure with laser, drops or surgery in the operating room.
Initial Treatment of Glaucoma: Laser or Drops?
As the first, and hopefully only, treatment for your glaucoma, you may choose to lower the eye’s pressure with laser or drops. The idea of having a laser makes many people nervous, and drops is certainly a legitimate way to go. Most ophthalmologists still have patients try multiple drops before going with laser, rather than using it as first-line treatment.
Glaucoma drops are for life. You will need to use them once or twice per day, every day, which is one more thing you have to remember. Many studies have shown that most patients are not able or willing to use the drops consistently, as directed, over the long haul. Imperfect drop-taking is a risk for your getting more glaucoma damage to your optic nerves.
Glaucoma drops can be expensive. The ones that work the best for most people are the most expensive.
Glaucoma drops have side-effects, even if you are not aware of them. They cause changes to the eye’s surface, increasing dryness. If you need surgery or laser later on because the drops don’t work adequately, being on drops for years makes it less likely the procedure will work.
The laser is an office procedure, done at a slit lamp, similar to the instrument we use to do your exam. It doesn’t hurt. You don’t need to change clothes or mind your activity afterward. There is a little redness and discomfort for a few days after. The laser works about 75% of the time — in about 25% it has no effect, in which case we would start drops. If the laser lowers your pressure but not quite all the way, it may have at least allowed us to have you use a less expensive drop or fewer drops than we would have done without the laser.
The downside to laser? Very rarely, it can make the eye’s pressure go up, rather than down. Dr. Lander has done laser trabeculoplasies since 1981 and has seen this happen once.
If you would like to learn more about the laser procedure, look on the internet under “selective laser trabeculoplasty.” Certainly, feel free to ask us any questions about it.
What is the risk of going blind?
That depends on how advanced your glaucoma is at the time it is discovered and how conscientious you are about taking care of it. If you are on drops, it is very important that you take them consistently. If you haven’t been taking the drops as you should, tell the doctor – we will work out a treatment plan that you can do, and we promise not to scold! Also, be sure to come in for regular checks, so that we can see if the treatment is working, and we can see if the damage to the optic nerves is getting worse. If you follow the treatment, we can prevent the glaucoma damage from getting worse the great majority of the time.
Drops
Most glaucoma patients need or choose drops. There are six major classes of them, and each one lowers the pressure by a different means than the others. If you are on drops, it is very important that you take them consistently. If you haven’t been taking the drops as you should, tell the doctor – we will work out a treatment plan that you can do. If you have trouble instilling drops, we can show you easy ways to do it.
Selective Laser Trabeculoplasty
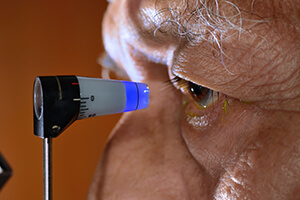 Selective laser trabeculoplasty (SLT) is a laser surgical procedure used to lower intraocular pressure (IOP) of patients with open-angle glaucoma. SLT is used to treat the eye’s drainage system, known as the trabecular meshwork – the drain that surrounds the iris. Treating this area of the eye’s natural drainage system improves the flow of fluid out of the eye, helping to lower the pressure.
Selective laser trabeculoplasty (SLT) is a laser surgical procedure used to lower intraocular pressure (IOP) of patients with open-angle glaucoma. SLT is used to treat the eye’s drainage system, known as the trabecular meshwork – the drain that surrounds the iris. Treating this area of the eye’s natural drainage system improves the flow of fluid out of the eye, helping to lower the pressure.
The laser used in SLT is very low-powered. It treats specific cells selectively, leaving untreated portions of the trabecular meshwork intact. It causes no demonstrable damage to the eye’s drain, unlike the older argon laser. For this reason SLT, unlike other types of laser surgery, may be safely repeated.
SLT is typically performed in the ophthalmologist’s (Eye M.D.’s) office or an outpatient surgery center. The procedure usually takes about five minutes. First, anesthetic drops are placed in your eye. The laser machine looks similar to the examination microscope that your doctor uses to look at your eyes at each office visit.
You will experience a flash of light with each laser application. Most people are comfortable and do not experience any significant pain during the surgery, although some may feel a little pressure.
Patients can resume normal daily activities the day of laser surgery. You will need to use eye drops after the procedure for a few days to maximize the laser’s effect.
It will take several weeks to determine how much SLT lowered your eye pressure. You may require additional laser, drops or glaucoma drainage surgery to lower the pressure, if it is not sufficiently lower after the first laser treatment.
In some, the laser is recommended as first-line therapy in order to avoid using drops. In others, it is used to make the drops the patient takes work better. In still others, SLT is used to avoid adding drops to the current drop regimen.
When your glaucoma is first diagnosed, you may be given the option of treatment with drops or laser. The advantage to laser is that, if it works, you can avoid taking drops for the rest of your life, avoiding the expense, effort and possible side effects of drops. SLT works about 75% of the time, on average. If it does not, drops will work just as well as if you never had the laser.
While some people may experience side effects from medications or surgery, the risks associated with these side effects should be balanced against the greater risk of leaving glaucoma untreated and losing your vision.
Peripheral Iridotomy
If your ophthalmologist (Eye M.D.) or optometrist suspects that you have “narrow” or “closed” angles, this means that the drainage channel of your eye is blocked or nearly blocked by the iris, the colored part of your eye. This can cause elevated intraocular pressure and subsequent vision loss. This is called angle-closure glaucoma.
An attack of acute angle-closure glaucoma is marked by sudden onset of very high eye pressure and complete blockage of the drain. Symptoms include pain, red-eye, and decreased vision. Here, the laser is done as an emergency procedure after the IOL is lowered in the emergency room. The eye pressure can also rise gradually (chronic angle-closure glaucoma)–you would have no symptoms at all. Most often, peripheral iridotomies are done when your eye doctor discovers angle closure on exam.
To treat angle-closure glaucoma, your ophthalmologist will perform a peripheral iridotomy (PI), creating a hole in the iris (the colored part of the eye) using a laser. This opening is typically so small that it cannot be seen with the naked eye. The opening in the iris allows fluid to flow from behind the iris through the opening, allowing the iris to fall back into a more normal position, opening the drain.
This laser treatment is performed in the ophthalmologist’s office. The treatment will not improve your vision but prevents vision loss from angle-closure glaucoma. Side effects of the treatment are unusual and include a temporary rise in intraocular pressure and inflammation. Sometimes, light can come through the hole and cause glare. If this occurs and it does not go away on its own, it can be eliminated by various means.
Non-laser surgery
Surgery in the operating room is usually tried only after laser and drops have proven to not lower the pressure adequately. The commonest one is a trabeculectomy, in which a new drain is created. With a seton an artificial drain is placed in the eye. Much talked about nowadays is MIGS, minimally-invasive glaucoma surgery. These various procedures involve surgery on the eye’s drain directly and are usually done at the time of cataract surgery. Most of these are in evolution and they don’t lower the pressure as well as a trabeculectomy or seton. Still, MIGS can be appropriate for some people.

